Human Skeleton

WELCOME TO STRONTIUM FOR BONES BLOG
Have you experienced negative, and even dangerous, side effects from Fosamax (alendronate), Boniva (ibandronate), Actonel (risedronate), Reclast (zoledronic acid), Prolia (denosumab), Forteo (teriparatide), Tymlos (abaloparatide), or other drugs prescribed for osteoporosis? If you have, then rest assured there is a safe, effective treatment for this condition. Strontium, primarily in the form of strontium citrate, is taken orally once a day.
Visitors to my blog can leave comments or ask questions and can remain anonymous, if they wish. Their comments are relayed to my g-mail inbox. Below each post, the number of comments for that post is cited and underlined because it is a link. By clicking on that link below any post, a window opens so that a visitor can leave a comment. Ideally, visitors leave comments on posts most relevant to their comments. All comments to my posts are moderated by me.
Browse the posts and visit the link library of references.
Visitors to my blog can leave comments or ask questions and can remain anonymous, if they wish. Their comments are relayed to my g-mail inbox. Below each post, the number of comments for that post is cited and underlined because it is a link. By clicking on that link below any post, a window opens so that a visitor can leave a comment. Ideally, visitors leave comments on posts most relevant to their comments. All comments to my posts are moderated by me.
Browse the posts and visit the link library of references.
Blog Archive
Friday, December 23, 2011
Effects of Strontium Ranelate on Spinal Osteoarthritis Progression
In “Effects of strontium ranelate on spinal osteoarthritis progression,” published in Ann Rheum Dis 2008;67:335-339, O Bruyere et al aimed to determine whether a three-year treatment with strontium ranelate could delay the progression of spinal osteoarthritis (OA).
This study was a post-hoc analysis of pooled data from the Spinal Osteoporosis Therapeutic Intervention (SOTI) and TReatment Of Peripheral OSteoporosis (TROPOS) trials performed on 1,105 women with osteoporosis and concomitant radiological spinal OA at baseline, and for whom lumbar x-rays were available at baseline and over the three-year treatment period. The presence and severity of osteophytes, disc space narrowing and sclerosis in the lumbar intervertebral spaces was graded, and an overall OA score was calculated for each intervertebral space. Back pain (measured on a five-point Likert scale only in SOTI) and health-related quality of life (SF-36 questionnaire) were assessed at baseline and after three years. Patients who suffered an incident or progressive vertebral fracture during the study were excluded from the analysis.
The proportion of patients with worsening overall spinal OA score was reduced by 42% in the strontium ranelate group, compared with placebo. Significantly more patients in the strontium ranelate group experienced an improvement in back pain after three years, compared with placebo, while no significant difference was observed in terms of health-related quality of life between these patient groups.
The researchers concluded that strontium ranelate could reduce the progression of the radiographic features of spinal osteoarthritis (OA) and back pain in women with osteoporosis and prevalent spinal OA. http://ard.bmj.com/content/67/3/335.abstract.
Friday, September 30, 2011
Supplements For Bone Health
On August 5, 2010, I posted “My Daily Supplements,” a list of the many supplements I take. You can access it at http://strontiumforbones.blogspot.com/search?updated-max=2010-08-21T15%3A28%3A00-04%3A00&max-results=6. Here are the three supplements I take specifically for osteoporosis and to which I attribute my significant gain in bone mineral density. The multivitamin is for general health, but, with 1000 IU vitamin D3, 200 mg calcium, 100 mg magnesium and 80 mcg vitamin K, it is an important part of my bone-building strategy. This list may help you get started on your own supplement program.
Because each one of us is unique, each will have to individually tailor his/her own program. Some people, for example, will need much more vitamin D3 than the 1000 IU I take. If your blood calcium level is low and/or your 25-hyroxy vitamin D test is low, and/or you live in a northern climate or an area of high smog density where your sun exposure is limited, you may have to take much higher vitamin D dosages. Corticosteroids, diuretics, anticonvulsants, and some heartburn medications may interfere with vitamin D. If you take any of these medicines, you may need to increase your vitamin D intake. I spend considerable time outdoors in a southern climate and my blood calcium levels tend to run high normal; therefore, 1000 IU vitamin D3 is plenty for me.
Doctor’s Best Strontium Bone Maker, 1944 mg strontium citrate, 680 mg elemental strontium in two capsules. I buy this at www.iherb.com.
Nature Made Multi For Her 50+ (contains 22 key nutrients, including 1000 IU vitamin D3, 200 mg calcium, 100 mg magnesium, 80 mcg vitamin K, 2500 IU vitamin A with 60% as beta carotene, 25 mcg vitamin B12, 180 mg vitamin C, 60 IU vitamin E, 15 mg zinc, 70 mcg selenium). I buy this at www.walgreens.com when they have two-for-one specials. Walgreens drugstores have the same specials.
Kal Extra-Strength Calcium Magnesium (I take one tablet, which contains 500 mg calcium and 250 mg magnesium.) The multivitamin listed above contains 200 mg calcium and 100 mg magnesium. I get approximately 500 mg calcium from food to total the 1200 mg recommended for a woman over 50 years old. I do eat dairy products. I am currently buying this supplement at www.vitaminshoppe.com.
Because each one of us is unique, each will have to individually tailor his/her own program. Some people, for example, will need much more vitamin D3 than the 1000 IU I take. If your blood calcium level is low and/or your 25-hyroxy vitamin D test is low, and/or you live in a northern climate or an area of high smog density where your sun exposure is limited, you may have to take much higher vitamin D dosages. Corticosteroids, diuretics, anticonvulsants, and some heartburn medications may interfere with vitamin D. If you take any of these medicines, you may need to increase your vitamin D intake. I spend considerable time outdoors in a southern climate and my blood calcium levels tend to run high normal; therefore, 1000 IU vitamin D3 is plenty for me.
Doctor’s Best Strontium Bone Maker, 1944 mg strontium citrate, 680 mg elemental strontium in two capsules. I buy this at www.iherb.com.
Nature Made Multi For Her 50+ (contains 22 key nutrients, including 1000 IU vitamin D3, 200 mg calcium, 100 mg magnesium, 80 mcg vitamin K, 2500 IU vitamin A with 60% as beta carotene, 25 mcg vitamin B12, 180 mg vitamin C, 60 IU vitamin E, 15 mg zinc, 70 mcg selenium). I buy this at www.walgreens.com when they have two-for-one specials. Walgreens drugstores have the same specials.
Kal Extra-Strength Calcium Magnesium (I take one tablet, which contains 500 mg calcium and 250 mg magnesium.) The multivitamin listed above contains 200 mg calcium and 100 mg magnesium. I get approximately 500 mg calcium from food to total the 1200 mg recommended for a woman over 50 years old. I do eat dairy products. I am currently buying this supplement at www.vitaminshoppe.com.
Tuesday, September 27, 2011
New BONIVA Advertisement Features Correction
Have you seen the latest BONIVA ad? Apparently, the Food and Drug Administration (FDA) has forced Roche Therapeutics Inc. to recant a previous unsubstantiated claim about their product, which contains ibandronate sodium, a bisphosphonate. I saw this ad in the September 25, 2011, Parade magazine, which is included with my Sunday newspaper. The title and first two paragraphs of the advertisement concern the correction:
“An important correction from BONIVA for women with postmenopausal osteoporosis”
“You may have seen an ad about BONIVA for the treatment and prevention of postmenopausal osteoporosis that may have given you the wrong impression. Our ads stated that ‘After one year on BONIVA, 9 out of 10 women stopped and reversed their bone loss.’ The FDA has found that there is not enough evidence to support this statement and wants us to clear up any misunderstanding you may have had about these ads and make sure you have the correct information about BONIVA.”
“BONIVA has not been proven to stop and reverse bone loss in 9 out of 10 women and is not a cure for postmenopausal osteoporosis. BONIVA has been shown to help increase bone mass and help reduce the chance of having a spinal fracture (break). We encourage all patients to discuss their treatment with their healthcare provider. Only your doctor can determine if BONIVA is right for you.”
“An important correction from BONIVA for women with postmenopausal osteoporosis”
“You may have seen an ad about BONIVA for the treatment and prevention of postmenopausal osteoporosis that may have given you the wrong impression. Our ads stated that ‘After one year on BONIVA, 9 out of 10 women stopped and reversed their bone loss.’ The FDA has found that there is not enough evidence to support this statement and wants us to clear up any misunderstanding you may have had about these ads and make sure you have the correct information about BONIVA.”
“BONIVA has not been proven to stop and reverse bone loss in 9 out of 10 women and is not a cure for postmenopausal osteoporosis. BONIVA has been shown to help increase bone mass and help reduce the chance of having a spinal fracture (break). We encourage all patients to discuss their treatment with their healthcare provider. Only your doctor can determine if BONIVA is right for you.”
Labels:
bisphosphonate,
bone loss,
Boniva,
ibandronate sodium
Tuesday, September 13, 2011
Antiresorptive, Anabolic, And Dual-Action Osteoporosis Drugs
Osteoporosis drugs can be divided into three categories: antiresorptive drugs that slow bone breakdown (resorption), anabolic drugs that build new bone, and dual-action drugs that both slow bone resorption and build new bone. Most approved osteoporosis drugs are antiresorptive. These slow bone loss and help fill in the remodeling spaces. All antiresorptive agents reduce the risk of vertebral (spinal) fractures and reduce markers of bone turnover. These markers are substances in the blood and urine that reflect the activity of the bone cells involved in breakdown and formation.
Antiresorptive medications include bisphosphonates, selective estrogen receptor modulators (SERMs), hormone replacement therapy (HRT), and calcitonin. Bisphosphonates include alendronate (Fosamax), risedronate (Actonel), ibandronate (Boniva), and zoledronic acid (Reclast). The only approved SERM is raloxifene (Evista). HRT includes several agents: Premarin, Prempro, Estrace, Estraderm, and Climara. Calcitonin is a polypeptide hormone secreted by the parafollicular cells of the thyroid gland in mammals and by the ultimobranchial gland of birds and fish. Miacalcin® (calcitonin-salmon) Nasal Spray is a synthetic polypeptide of 32 amino acids in the same linear sequence that is found in calcitonin of salmon origin. Miacalcin is also available as an injection.
The newest drug in the antiresorptive category is denosumab (Prolia), an injection administered subcutaneously once every six months. Prolia binds to RANKL, a transmembrane or soluble protein essential for the formation, function, and survival of osteoclasts, the cells responsible for bone resorption. Prolia prevents RANKL from activating its receptor, RANK, on the surface of osteoclasts and their precursors. Prevention of the RANKL/RANK interaction inhibits osteoclast formation, function, and survival, thereby decreasing bone resorption and increasing bone mass and strength in both cortical and trabecular bone.
In clinical trials in women with postmenopausal osteoporosis, treatment with Prolia resulted in significant suppression of bone remodeling as evidenced by markers of bone turnover and bone histomorphometry. The significance of these findings and the effect of long-term treatment with Prolia are unknown. The long-term consequences of the degree of suppression of bone remodeling observed with Prolia may contribute to adverse outcomes such as osteonecrosis of the jaw, atypical fractures, and delayed fracture healing.
Antiresorptives do not build bone beyond what is produced to help fill the remodeling spaces. Bone-building (anabolic) drugs, on the other hand, stimulate bone formation by increasing the activity of the cells known as osteoblasts. The only such medication approved in the U.S.A. for treating osteoporosis is teriparatide (Forteo), a form of human parathyroid hormone (PTH). The drug comes as a daily injection, which can be self-administered. PTH produces larger increases in BMD than antiresorptives do. It also improves bone microarchitecture. However, it is prescribed for no more than about two years because its long-term safety and efficacy are unknown. Most experts recommend that antiresorptive drugs be stopped during PTH therapy and restarted after the course of PTH is complete.
Strontium ranelate is a compound that incorporates the element strontium, which is found in trace amounts throughout the skeleton. Results from Phase III trials conducted by French researchers suggest that strontium ranelate may reduce vertebral fractures about as well as bisphosphonates. The drug is believed to work by decreasing bone breakdown and increasing bone buildup. This prescription drug is not available in the U.S.A., but strontium citrate can be purchased as a supplement.
My opinion is that the antiresorptive drugs are flawed models as osteoporosis drugs. If we keep slowing bone breakdown without building new bone, we eventually end up with very old, weak bones. Long-term suppression of bone remodeling by Fosamax and other bisphosphonates has led to osteonecrosis of the jaw and atypical femur fractures in some patients. Better models are bone-building (anabolic) drugs (i.e. Forteo) and dual-action agents (i.e. strontium ranelate, strontium citrate) that decrease bone breakdown and increase bone buildup.
http://www.health.harvard.edu/newsweek/Update_on_osteoporosis_drugs.htm
http://www.rxlist.com/miacalcin-drug.htm
http://www.rxlist.com/prolia-drug.htm
Antiresorptive medications include bisphosphonates, selective estrogen receptor modulators (SERMs), hormone replacement therapy (HRT), and calcitonin. Bisphosphonates include alendronate (Fosamax), risedronate (Actonel), ibandronate (Boniva), and zoledronic acid (Reclast). The only approved SERM is raloxifene (Evista). HRT includes several agents: Premarin, Prempro, Estrace, Estraderm, and Climara. Calcitonin is a polypeptide hormone secreted by the parafollicular cells of the thyroid gland in mammals and by the ultimobranchial gland of birds and fish. Miacalcin® (calcitonin-salmon) Nasal Spray is a synthetic polypeptide of 32 amino acids in the same linear sequence that is found in calcitonin of salmon origin. Miacalcin is also available as an injection.
The newest drug in the antiresorptive category is denosumab (Prolia), an injection administered subcutaneously once every six months. Prolia binds to RANKL, a transmembrane or soluble protein essential for the formation, function, and survival of osteoclasts, the cells responsible for bone resorption. Prolia prevents RANKL from activating its receptor, RANK, on the surface of osteoclasts and their precursors. Prevention of the RANKL/RANK interaction inhibits osteoclast formation, function, and survival, thereby decreasing bone resorption and increasing bone mass and strength in both cortical and trabecular bone.
In clinical trials in women with postmenopausal osteoporosis, treatment with Prolia resulted in significant suppression of bone remodeling as evidenced by markers of bone turnover and bone histomorphometry. The significance of these findings and the effect of long-term treatment with Prolia are unknown. The long-term consequences of the degree of suppression of bone remodeling observed with Prolia may contribute to adverse outcomes such as osteonecrosis of the jaw, atypical fractures, and delayed fracture healing.
Antiresorptives do not build bone beyond what is produced to help fill the remodeling spaces. Bone-building (anabolic) drugs, on the other hand, stimulate bone formation by increasing the activity of the cells known as osteoblasts. The only such medication approved in the U.S.A. for treating osteoporosis is teriparatide (Forteo), a form of human parathyroid hormone (PTH). The drug comes as a daily injection, which can be self-administered. PTH produces larger increases in BMD than antiresorptives do. It also improves bone microarchitecture. However, it is prescribed for no more than about two years because its long-term safety and efficacy are unknown. Most experts recommend that antiresorptive drugs be stopped during PTH therapy and restarted after the course of PTH is complete.
Strontium ranelate is a compound that incorporates the element strontium, which is found in trace amounts throughout the skeleton. Results from Phase III trials conducted by French researchers suggest that strontium ranelate may reduce vertebral fractures about as well as bisphosphonates. The drug is believed to work by decreasing bone breakdown and increasing bone buildup. This prescription drug is not available in the U.S.A., but strontium citrate can be purchased as a supplement.
My opinion is that the antiresorptive drugs are flawed models as osteoporosis drugs. If we keep slowing bone breakdown without building new bone, we eventually end up with very old, weak bones. Long-term suppression of bone remodeling by Fosamax and other bisphosphonates has led to osteonecrosis of the jaw and atypical femur fractures in some patients. Better models are bone-building (anabolic) drugs (i.e. Forteo) and dual-action agents (i.e. strontium ranelate, strontium citrate) that decrease bone breakdown and increase bone buildup.
http://www.health.harvard.edu/newsweek/Update_on_osteoporosis_drugs.htm
http://www.rxlist.com/miacalcin-drug.htm
http://www.rxlist.com/prolia-drug.htm
Friday, August 12, 2011
Bone Remodeling
Bone remodeling is the replacement of old bone tissue by new bone tissue. This process, which mainly occurs in the adult skeleton to maintain bone mass, involves the coupling of bone formation and bone resorption and consists of five phases:
1. Activation: preosteoclasts are stimulated and differentiate under the influence of cytokines and growth factors into mature active osteoclasts
2. Resorption: osteoclasts digest mineral matrix (old bone)
3. Reversal: end of resorption
4. Formation: osteoblasts synthesize new bone matrix
5. Quiescence: osteoblasts become resting bone lining cells on the newly formed bone surface
http://www.iofbonehealth.org/health-professionals/about-osteoporosis/basic-bone-biology.html
1. Activation: preosteoclasts are stimulated and differentiate under the influence of cytokines and growth factors into mature active osteoclasts
2. Resorption: osteoclasts digest mineral matrix (old bone)
3. Reversal: end of resorption
4. Formation: osteoblasts synthesize new bone matrix
5. Quiescence: osteoblasts become resting bone lining cells on the newly formed bone surface
http://www.iofbonehealth.org/health-professionals/about-osteoporosis/basic-bone-biology.html
Friday, July 22, 2011
Strontium Ranelate And Risk Of Vertebral Fractures In Frail Osteoporotic Women
Data were obtained from the SOTI (Spinal Osteoporosis Therapeutic Intervention) and TROPOS (Treatment Of Peripheral Osteoporosis) studies which randomized participants to receive either strontium ranelate or placebo over three years. The study identified 2346 robust, 2472 intermediate and 264 frail women. At three years, the risk for vertebral fractures was reduced by 30% in the robust, by 45% in the intermediate, and by 58% in the frail patients compared to those assigned to placebo. Risk of vertebral fracture was reduced within one year in all three groups.
This study was published by Rolland Y, Van Kan GA, Gillette-Guyonnet S, Roux C, Boonen S, and Vellas B in Bone 2011;48:332-8.
This study was published by Rolland Y, Van Kan GA, Gillette-Guyonnet S, Roux C, Boonen S, and Vellas B in Bone 2011;48:332-8.
Tuesday, July 19, 2011
The Effect Of Bone Strontium On BMD Differs For Different DXA Equipment
Osteoporotic patients treated with strontium ranelate show relatively large increases in bone mineral density (BMD) measured by dual-energy X-ray absorptiometry (DXA) due to the replacement of some of the calcium atoms in bone by strontium. A study by Pors Nielsen and colleagues reported that replacement of 1% of calcium atoms by strontium causes a 10% increase in BMD. The ratio of the percentage increase in BMD to the molar percentage of strontium in bone is referred to as the strontium ratio. Theoretically it is expected that the strontium ratio should vary between different manufacturers' DXA equipment depending on the effective photon energy of the device.
In this study the researchers reported theoretical estimates of the strontium ratio for two axial DXA systems and two peripheral DXA devices based on their broad spectrum X-ray emission. The theoretical figures were verified in an experimental study in which the strontium ratio for each device was measured using phantoms containing mixtures of hydroxyapatite and strontium hydrogen-phosphate. The theoretical values of the strontium ratio were 11.0 for the Hologic Discovery, 9.9 for the GE-Lunar Prodigy, 9.1 for the Demetech Calscan, and 8.5 for the Osteometer Dexacare G4. Experimental results were 11.2 for the Discovery, 9.9 for the Prodigy, 8.6 for the Calscan and 6.3 for the Dexacare G4. The results confirm that the effect of bone strontium on BMD measurements is different for different DXA systems. In the future it might be possible to exploit this effect to make a non-invasive estimate of average bone strontium content in groups of patients receiving strontium medication for osteoporosis.
Liao J, Blake GM, McGregor AH, Patel R. Bone. 2010 Nov; 47(5):882-7. Epub 2010 Aug 10
http://www.ncbi.nlm.nih.gov/pubmed/20699129
In this study the researchers reported theoretical estimates of the strontium ratio for two axial DXA systems and two peripheral DXA devices based on their broad spectrum X-ray emission. The theoretical figures were verified in an experimental study in which the strontium ratio for each device was measured using phantoms containing mixtures of hydroxyapatite and strontium hydrogen-phosphate. The theoretical values of the strontium ratio were 11.0 for the Hologic Discovery, 9.9 for the GE-Lunar Prodigy, 9.1 for the Demetech Calscan, and 8.5 for the Osteometer Dexacare G4. Experimental results were 11.2 for the Discovery, 9.9 for the Prodigy, 8.6 for the Calscan and 6.3 for the Dexacare G4. The results confirm that the effect of bone strontium on BMD measurements is different for different DXA systems. In the future it might be possible to exploit this effect to make a non-invasive estimate of average bone strontium content in groups of patients receiving strontium medication for osteoporosis.
Liao J, Blake GM, McGregor AH, Patel R. Bone. 2010 Nov; 47(5):882-7. Epub 2010 Aug 10
http://www.ncbi.nlm.nih.gov/pubmed/20699129
Thursday, June 23, 2011
Dietary Calcium Intake And Risk Of Fracture And Osteoporosis
The optimal level of calcium intake to compensate for skeletal calcium losses and to prevent osteoporosis and fractures remains unclear. This is reflected by the wide range of daily calcium recommendations for individuals older than 50 years: at present 700 mg in the UK, 800 mg in Scandinavia, 1200 mg in the United States, and 1300 mg in Australia and New Zealand.
The findings of a large Swedish study recently published in the British Medical Journal show an association between a low habitual dietary calcium intake (below 751 mg per day for women) and an increased risk of fractures and of osteoporosis. Above this base level, only minor differences in risk were observed. The highest reported calcium intake (>1137 mg) did not further reduce the risk of fractures of any type, or of osteoporosis, but was associated with a higher rate of hip fracture.
Eva Warensjö, et al. BMJ. 2011; 342: d1473.
Published online 2011 May 24. doi: 10.1136/bmj.d1473.
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3101331/
The findings of a large Swedish study recently published in the British Medical Journal show an association between a low habitual dietary calcium intake (below 751 mg per day for women) and an increased risk of fractures and of osteoporosis. Above this base level, only minor differences in risk were observed. The highest reported calcium intake (>1137 mg) did not further reduce the risk of fractures of any type, or of osteoporosis, but was associated with a higher rate of hip fracture.
Eva Warensjö, et al. BMJ. 2011; 342: d1473.
Published online 2011 May 24. doi: 10.1136/bmj.d1473.
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3101331/
Labels:
dietary calcium,
fracture risk,
hip fracture,
osteoporosis
Thursday, April 21, 2011
Drugs Associated With Increased Bone Loss And Fracture Risk
"Certain drugs (e.g., glucocorticoids, carbamazepine, phenytoin, valproic acid, lithium, depot medroxyprogesterone, chemotherapeutic agents, and long-term heparin therapy) are known to be associated with increases in bone loss or fracture rate. Thiazolidinediones are the newest addition to this list, as recent clinical trials have reported increased fracture rates in patients receiving these drugs for the treatment of type 2 diabetes mellitus."
"Pioglitazone and rosiglitazone, the two currently available thiazolidinediones, accounted for nearly one quarter of the antidiabetic drugs prescribed in the United States in 2004 and 2005. In 2008, both pioglitazone (8th) and rosiglitazone (98th) ranked within the top 100 prescription drug sales in the United States. This widespread use has exposed many postapproval adverse effects, including bone changes and fractures."
The entire article can be read at:
http://www.medscape.com/viewarticle/725156
Bone Loss and Fracture Risk Associated with Thiazolidinedione Therapy
Daniel M. Riche, Pharm.D.; S. Travis King, Pharm.D.
Posted: 10/05/2010; Pharmacotherapy
"Pioglitazone and rosiglitazone, the two currently available thiazolidinediones, accounted for nearly one quarter of the antidiabetic drugs prescribed in the United States in 2004 and 2005. In 2008, both pioglitazone (8th) and rosiglitazone (98th) ranked within the top 100 prescription drug sales in the United States. This widespread use has exposed many postapproval adverse effects, including bone changes and fractures."
The entire article can be read at:
http://www.medscape.com/viewarticle/725156
Bone Loss and Fracture Risk Associated with Thiazolidinedione Therapy
Daniel M. Riche, Pharm.D.; S. Travis King, Pharm.D.
Posted: 10/05/2010; Pharmacotherapy
Monday, February 28, 2011
Systematic Treatment After Successful Surgical Treatment for Primary Hyperparathyroidism With Strontium Ranelate
Patients with primary hyperparathyroidism (pHPT) with osteopenia or osteoporosis are treated with strontium ranelate/Ca+Vitamin-D or placebo/Ca+Vitamin D after successful surgical treatment of pHPT. This clinical trial is currently recruiting participants. ClinicalTrials.gov processed this record on February 27, 2011.
The chronic excessive hypersecretion of parathyroid hormone (PTH) has significant impact on bone remodeling. In primary hyperparathyroidism (pHPT) bone turnover is increased, resulting in a higher resorption of bone and thus loss of bone density.
After successful surgical treatment of pHPT, bone metabolism switches from catabolic state to anabolic state again. However, studies show that postmenopausal women in particular regain significantly less BMD and often suffer from osteopenia or osteoporosis. The hypothesis is that strontium ranelate/Ca + Vitamin-D helps to regain bone mass in patients with osteopenia or osteoporosis after successful parathyroidectomy for pHPT and results in higher gain of BMD than placebo-treated patients.
Eligibility Requirements: 18 Years and older, either gender, biochemically proven pHPT and PTX planned, osteopenia (t-score < -1 and > -2.5) or osteoporosis (t-score ≤ -2.5) according to WHO Criteria
Medical University Vienna, General Hospital Vienna, Vienna, Austria, 1090
Contact: Bruno Niederle, Prof., MD. at chir-endokrin@meduniwien.ac.at
Contact: Christian Scheuba, Prof., MD at christian.scheuba@meduniwien.ac.at
There is a long list of exclusion criteria and more information at:
http://www.clinicaltrials.gov/ct2/show/NCT01222026?term=strontium+AND+osteoporosis&rank=1
The chronic excessive hypersecretion of parathyroid hormone (PTH) has significant impact on bone remodeling. In primary hyperparathyroidism (pHPT) bone turnover is increased, resulting in a higher resorption of bone and thus loss of bone density.
After successful surgical treatment of pHPT, bone metabolism switches from catabolic state to anabolic state again. However, studies show that postmenopausal women in particular regain significantly less BMD and often suffer from osteopenia or osteoporosis. The hypothesis is that strontium ranelate/Ca + Vitamin-D helps to regain bone mass in patients with osteopenia or osteoporosis after successful parathyroidectomy for pHPT and results in higher gain of BMD than placebo-treated patients.
Eligibility Requirements: 18 Years and older, either gender, biochemically proven pHPT and PTX planned, osteopenia (t-score < -1 and > -2.5) or osteoporosis (t-score ≤ -2.5) according to WHO Criteria
Medical University Vienna, General Hospital Vienna, Vienna, Austria, 1090
Contact: Bruno Niederle, Prof., MD. at chir-endokrin@meduniwien.ac.at
Contact: Christian Scheuba, Prof., MD at christian.scheuba@meduniwien.ac.at
There is a long list of exclusion criteria and more information at:
http://www.clinicaltrials.gov/ct2/show/NCT01222026?term=strontium+AND+osteoporosis&rank=1
Subscribe to:
Posts (Atom)
Wandering Skeleton

Artist: Joel Hoekstra
Osteoporotic Bone
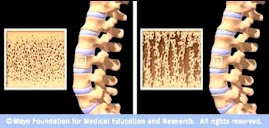
Source: www.mayoclinic.com
How Strontium Builds Bones
Strontium is a mineral that tends to accumulate in bone. Studies have shown that oral doses of strontium are a safe and effective way to prevent and reverse osteoporosis. Doses of 680 mg per day appear to be optimal. See my "For More Information About Strontium" links section.
Osteoporosis is caused by changes in bone production. In healthy young bones there is a constant cycle of new bone growth and bone removal. With age, more bone is removed and less new bone is produced. The bones become less dense and thus more fragile.
Scientists believe that strontium works in two ways. It may stimulate the replication of pre-osteoblasts, leading to an increase in osteoblasts (cells that build bone). Strontium also directly inhibits the activity of osteoclasts (cells that break down bone). The result is stronger bones.
When taking strontium, be sure to take 1200 mg calcium, 1000 IU vitamin D3, and 500 mg magnesium daily. It is best to take strontium late at night on an empty stomach. Calcium and strontium may compete with each other for absorption if taken together.
Osteoporosis is caused by changes in bone production. In healthy young bones there is a constant cycle of new bone growth and bone removal. With age, more bone is removed and less new bone is produced. The bones become less dense and thus more fragile.
Scientists believe that strontium works in two ways. It may stimulate the replication of pre-osteoblasts, leading to an increase in osteoblasts (cells that build bone). Strontium also directly inhibits the activity of osteoclasts (cells that break down bone). The result is stronger bones.
When taking strontium, be sure to take 1200 mg calcium, 1000 IU vitamin D3, and 500 mg magnesium daily. It is best to take strontium late at night on an empty stomach. Calcium and strontium may compete with each other for absorption if taken together.
For More Information about Strontium
- A Dose-response Study With Strontium Malonate
- A Review of the latest insights into the mechanism of action of strontium in bone
- Antifracture Efficacy Over 10 Years With Strontium Ranelate
- Combination of Micronutrients for Bone (COMB) Study: Bone Density after Micronutrient Intervention
- Echolight REMS Scan of Young, Normal Female
- Effect of bone strontium on BMD measurements
- Effect of Lumbar Scoliosis on DXA Results
- Effects of SrR on Calcium Metabolism
- Effects of strontium ions on growth and dissolution of hydroxyapatite and on bone mineral detection
- Influence of strontium on bone mineral density and bone mineral content measurements by dual X-ray absorptiometry
- Interpretation of BMD Scans in Patients Stopping Strontium
- Melatonin-micronutrients Osteopenia Treatment Study (MOTS)
- National Osteoporosis Foundation
- Osteoporosis And Bone Physiology
- Post-Marketing Assessment of the Safety of Strontium Ranelate
- PubMed Abstract On The SOTI Study
- PubMed Abstract On The TROPOS Study
- Strontium ranelate Aristo
- Strontium Ranelate For Spinal Osteoarthritis
- Strontium: Breakthrough Against Osteoporosis
- Summary Safety Review - Strontium
- The Effects of Strontium Ranelate on the Risk of Vertebral Fracture in Women with Postmenopausal Osteoporosis
- The Influence of Strontium on Bone Tissue Metabolism and Its Application in Osteoporosis Treatment
- Thirteen Key Diagnostic Tests