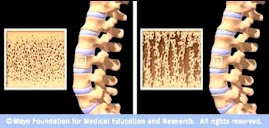
“Osteoporosis and resultant fractures of the spine, hip and
other sites are important public health problems with significant individual
and societal costs. The risk for osteoporotic fracture is based upon low bone
density and the presence of one or more clinical risk factors (see Table 1). A
history of fracture during adulthood or falls are important clinical factors in
determining the risk of future fracture; however, age is the most influential
risk factor, such that middle-aged adults with other risk factors are likely to
be at low absolute fracture risk in the medium term. Using these clinical risk
factors and BMD when available, fracture risk assessment tools (based upon data
collected from large prospective observational studies) have been developed to
estimate the 5–10 year probability of hip fracture and other fractures in
untreated patients. Clinicians should be aware that fracture risk can also be
estimated using the FRAX or Garvan tools without BMD data. Chronic
glucocorticoid use is an established risk factor for osteoporosis, with studies
showing that use of glucocorticoids leads to accelerated bone loss and an
increased risk of fracture. Other drugs are increasingly recognized as
potential causes of bone loss and fracture, particularly amongst predisposed
individuals….”
See the following link for more on other drugs that can
cause bone loss and fractures:
|
Table
1. Clinical risk factors for fracture
|
|
Advancing age
|
|
Previous fracture during adulthood
|
|
History of a fall or falls in the
past 12 months
|
|
Glucocorticoid therapy
|
|
Parental history of hip fracture
|
|
Low body weight
|
|
Current cigarette smoking
|
|
Excessive alcohol consumption
|
|
Medical diseases (e.g. rheumatoid
arthritis, hyperparathyroidism, coeliac disease, hypogonadism)
|
This introduction and table
appeared in “Adverse Skeletal Effects of Drugs – Beyond Glucocorticoids,” Susannah O'Sullivan, Andrew Grey, Clin
Endocrinol. 2015; 82(1):12-22.
http://www.medscape.com/viewarticle/837369?src=wnl_edit_tpal&uac=127701PY